William Pang
The success of dental procedures depends heavily on pain management. Local anesthetics have evolved from herbal remedies used by the Babylonians in 2250 B.C. to complex nerve blockade injections with synthetic compounds such as Lidocaine (Prichard). Modern anesthesia began with the discovery of ether in the 19th century. It has continued to evolve alongside dentistry, permitting the execution of procedures that would be otherwise too painful to tolerate. The modern dental professional has a spectrum of anesthetics within arm’s reach and must be well informed on the selection, delivery, and management of these compounds to ensure the safety and comfort of their patients.
Prior to the delivery of any local anesthetic, a layer of topical anesthetic is applied to the surrounding anatomy to minimize discomfort during the injection(s) of stronger local anesthetics. Topical anesthetics such as Benzocaine work by numbing the surface of the gingiva, or gums. Only the external part of the mucous membrane becomes desensitized while the teeth and underlying bony structures remain susceptible to pain signals (Scarlett). Typically, a sterile cotton swab is used to administer the topical agents.
After a brief latent period, a dental syringe can be loaded with the specified carpule, or cartridge containing the anesthetic. The injection releases the pharmacologic agent which blocks pain sensations in the area of the mouth that the procedure(s) will affect. Local anesthetics are classified based on their length of duration: short, moderate, or long. The most popular option is Lidocaine 2%, which has a moderate duration of 2 hours after a quick onset period of 2 minutes. On the other hand, Bupivacaine 0.25% has a long duration of up to 4 hours and a longer onset period of 5 minutes(Prichard). Usually, these compounds are combined with a vasoconstrictor, such as epinephrine, along with the active ingredient (i.e. Lidocaine 2% with Epinephrine 1:100,000) (Scarlett). The addition of epinephrine increases the duration of anesthesia by slowing the rate of vascular uptake (Jastak). Oftentimes, dentists use a variety of anesthetics for different parts of mouth. To avoid confusion, carpules are tagged with a colored band corresponding to their active ingredient.
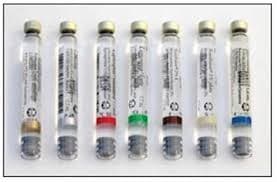
Fig. 1. The spectrum of colors are indicative of specific anesthetic agents.
Risks and Contraindications
Proper care and safety regulations must be followed to decrease the risk for infections as a result of accidental needlesticks. The most vulnerable period is post-injection, when the needle is contaminated with patient blood that may potentially carry blood borne pathogens such as HIV, HBV, and HCV. For safety purposes, the dentist should always assume all patients carry the aforementioned pathogens and exhibit the utmost caution when handling sharp objects such as a syringe. Furthermore, dental needles are single use only and must be immediately discarded in a special sharps container after they are used.
Besides the risk of needlesticks, there are contraindications associated with anesthetic use. A contraindication is a symptom that complicates and makes a treatment inadvisable. For example, cocaine users have an increased risk of dangerously elevated blood pressure and cardiac arrhythmias, when treated with injectable anesthetics. In addition, individuals who take certain antidepressants fare better with small doses of epinephrine as opposed to levonordefrin. Therefore, dentists must take into account each patient’s unique past and medical history, as well as lifestyle habits, in order to make the best judgement for them.

Fig. 2. Sharps containers have a thick outer layer and feature a one-way design that protects against removal of its contents.
New Delivery System
The traditional administration of local anesthetics with an aspirating dental syringe has undergone minimal innovation since its introduction in clinical practice. However, recent advancements in technology are changing the way dentistry is performed. Within the last decade, a new method of delivering local anesthetics has emerged – Single Tooth Anesthesia (STA). This system automatically calibrates and administers a precise injection rate (mL/sec) that is below the threshold for pain. A steady and slow controlled injection is most comfortable as it is less traumatic to surrounding tissues. However, even dentists with the finest manual dexterity skills will induce a degree of discomfort in their patients. The pain experienced from injections is derived from the injection rate. Thus, the STA’s novel delivery mechanism facilitates pain-free injections. In addition, the ingenious design features a flexible needle tip resembling a wand. Its innocuous appearance does not provoke the anxiety associated with the notoriously long aspirating needle, the cause of many dental phobias. Another benefit includes the delivery of two carpules of anesthetics without the removal and reinsertion of the needle (DiTolla). Finally, a foot pedal prompts the unit to begin delivery and absolves the burden of the dentist to simultaneously hold the syringe while performing the injection. This relieves unnecessary hand stress that plagued dentists in the past and over time will promote the longevity of the practice.
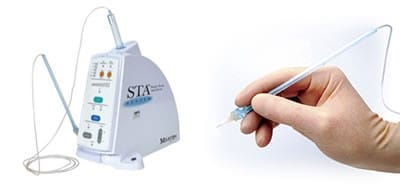
Fig. 3. The STA Wand System’s ergonomic design and computer-controlled dental injection improves comfort for both dentist and patient, respectively.
The introduction of local anesthesia has given patients access to a wide range of dental procedures. As more complex treatment modalities are pioneered, innovations in anesthesia and delivery devices must continue to emerge. Recent developments such as the STA are pushing the envelope of administration methods. Its success has inspired others to reimagine the stereotype of long needles and screams associated with the dentist’s office of yesteryear. The continuing trend in technological advances within local anesthesia will ultimately improve the efficiency, comfort, and safety of treatments performed on patients, ensuring better oral health and reducing dental phobia.